ICD-10 Diagnosis Codes:
H40.1211–Low-tension glaucoma, right eye, mild stage
H40.1212–Low-tension glaucoma, right eye, moderate stage
H40.1213–Low-tension glaucoma, right eye, severe stage
H40.1221–Low-tension glaucoma, left eye, mild stage
H40.1222–Low-tension glaucoma, left eye, moderate stage
H40.1223–Low-tension glaucoma, left eye, severe stage
H40.1231–Low-tension glaucoma, bilateral, mild stage
H40.1232–Low-tension glaucoma, bilateral, moderate stage
H40.1233–Low-tension glaucoma, bilateral, severe stage
Title
Low-Tension Glaucoma
Category
Glaucoma
Description
Low-tension glaucoma (e.g., normal-tension glaucoma) is defined as glaucoma where the intraocular pressure is never measured above 21 mm Hg.
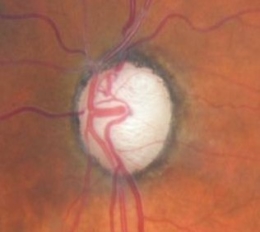
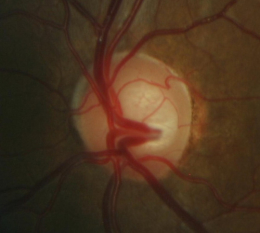
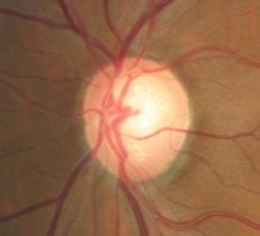
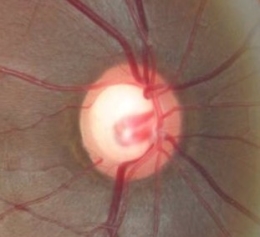
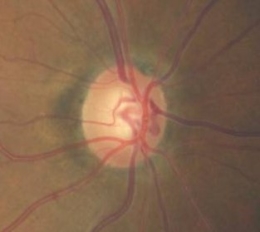
Glaucomatous Optic Atrophy
- Changes in coloration of the optic nerve
- Enlargement of the optic cup
- Wipe out of the neuroretinal rim
- Fallout of the retinal nerve fiber layer
For patients with normal-tension glaucoma, there remains some controversy on whether unphysiologic intraocular pressure is the dominant factor involved in developing glaucomatous optic atrophy or if there is a secondary component such as compromised blood flow to the optic nerve head.
Because of this, understanding normal-tension glaucoma from an oculosystemic perspective is best when deciding on treatment options that allow for neuro-protection of the optic nerve. Despite the etiology, normal-tension glaucoma has the same milestones of development as other types of open-angle glaucoma.
Normal-Tension Glaucoma vs Primary Open-Angle Glaucoma
- Sharper field loss in normal-tension glaucoma
- Shallower cupping in normal-tension glaucoma
- Larger overall disc area in normal-tension glaucoma
- Disc hemorrhages five-fold more prevalent in normal-tension glaucoma than primary open-angle glaucoma
- Higher and greater incidence of peripapillary atrophy and crescents in normal-tension glaucoma than primary open-angle glaucoma
Structural Damage to the Eye
- Atrophy of the optic nerve
- Acquired loss of retinal ganglion cells
Functional Damage to the Visual System
Associated visual field defects
- Reduction in retinal sensitivity
- Constriction of isopters
- Nasal steps
- Paracentral scotomas
- Arcuate scotomas
- Hemifield asymmetry
- Temporal changes in visual field patterns
- Loss of central acuity
Electrodiagnostic abnormalities
- Delayed peak times
- Reduced amplitudes
- Abnormal waveform morphology
Color vision abnormalities
- Acquired color vision defects
Pupillary reactivity abnormalities
- Relative afferent pupillary defect
The main goal in a patient with normal-tension glaucoma is to accomplish the following:
- Make a clinical diagnosis of normal-tension glaucoma
- Identify and exclude any oculosystemic conditions associated with normal-tension glaucoma
Patient History
- Patients will usually be asymptomatic in the early stages of glaucoma.
Intraocular Pressure
- Never measures above 21 mmHg
Gross Visual Fields
- Normal
- Constrictions
Pupillary Examination
- A relative afferent pupillary defect (RAPD) may be present if one eye is more affected than the other
External Ocular Examination with Biomicroscopy
- Normal
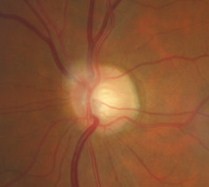
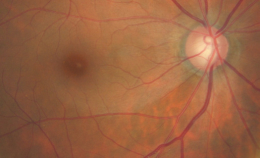
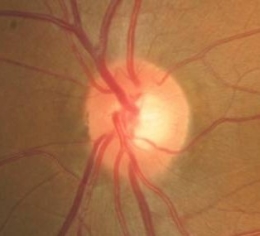
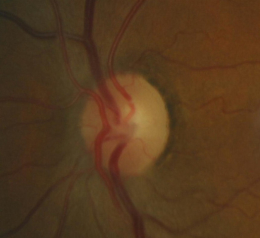
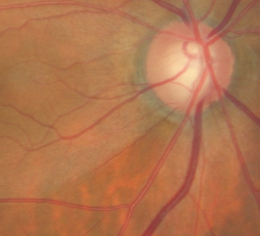
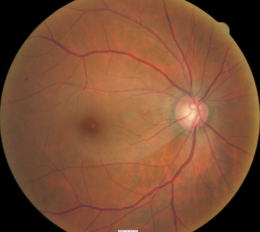
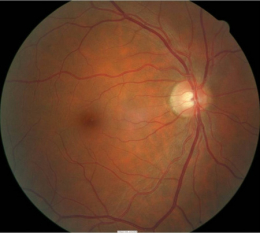
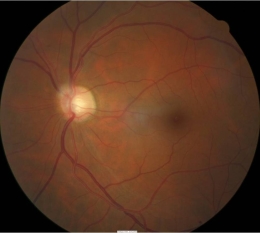
Ophthalmoscopic Examination
- Asymmetric optic disc cupping
- cup-to-disc ratio = .50/.40 in the right eye
- cup-to-disc ratio = .60/.60 in the left eye
- Inferior and superior focal optic disc notch in the left eye
- Pallor of the temporal neuroretinal rim in the left eye
Is the cupping physiologic or pathologic?
- Accurate visual fields as well as other optic nerve function and structure studies should identify truly diseased nerves
- Misdiagnosis of megalopapillae
Is the cupping progressive?
- Serial or sequential optic nerve function and structure studies will identify progression. There are a host of masquerading conditions that present with field defects (e.g., filted discs) that are non-progressive. Do not spend a lot of time trying to treat a non-progressive anomaly.
 |
 |
DIAGNOSTIC TESTS
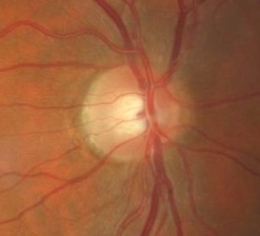
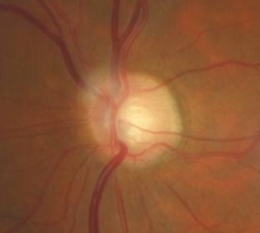
Fundus Photography
- To document the progress or lack of progress of macular degeneration
- To document the delivery of medical treatment
- To document the response to treatment
- To help plan a treatment program
- Fundus autofluorescence imaging can be used to detect structural abnormalities and predict functional deficits before standard color fundus photography
- Multi-spectral imaging with the Annidis RHA System can be used to detect structural abnormalities and predict functional deficits before standard color fundus photography
Extended Ophthalmoscopy
- xxx
- xxx
 |
 |
Medical Evaluation
- Vascular studies
- Blood glucose
- CBC (Hyperviscosity/ anemia)
- B12
- ANA
- ACE
- CXR
- FTA-ABS/ RPR
- Lyme
- Thyroid
- Mitochondrial DNA
- SPEP retinal antibodies
- Serum chemistries (lipids)
- ESR (erythrocyte sedimentation rate)
- Carotid blood flow studies
- Neuroimaging (if under age 65, rapidly progressing, unilateral, dyschromatopsia, acuity loss) of the orbits and chiasm
Be patient in making a diagnosis of normal-tension glaucoma. It should take at least 6-12 months in order to make the diagnosis when determining progression.
Normal-tension glaucoma is an acquired open-angle glaucoma. The disease can be classified by its Level of Control and its Category of Damage.
Levels of Glaucoma Control
Good Control
- Achievement of an intraocular pressure at or below the target pressure without significant adverse effects. Susequent observation confirms appropriateness of target pressure level by documenting lack of significant glaucomatous progression.
Borderline Control
- Achievement of an intraocular pressure near but higher than the target pressure, judged capable of inducing further glaucomatous damage.
Uncontrolled
- Intraocular pressure above the target pressure, judged capable of causing significant progressive glaucomatous damage
- Any evidence of glaucoma progression
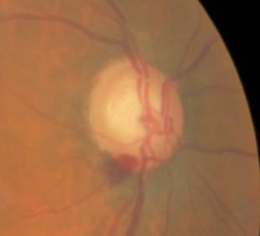
- Optic disc hemorrhage
- Reliable, reproducible, significant progression of visual field defects
- Progressive enlargement of the optic cup
- Progressive observable loss of the retinal nerve fiber layer
- Symptomatic decline in vision, consistent with glaucoma progression, otherwise unexplainable in a patient with moderate to advanced glaucoma
Category of Glaucoma Damage
Mild Damage — Visual Field
- No deteclable visual field defect
- Mild generalized reduction in retinal sensitivity
- Mild constriction of isopter
- Nasal step to 20 degrees
- Paracentral scotomas
Mild Damage — Optic Nerve
- No definite pathologic cupping
- Symmetric or vertically elongated cup enlargement
- Intact neuroretinal rim
- Previously observed optic disc hemorrhage
Moderate Damage — Visual Field
- Moderate generalized reduction in retinal sensitivity
- Moderate constriction of isopters, absolute defects within 9 degrees of fixation
Moderate Damage — Optic Nerve
- Enlarged optic cup
- Changes in coloration of the neuroretinal rim
- Sloped neuroretinal rim
- Focal optic disc notch
- Prominent lamina cribrosa
Advanced Damage — Visual Field
- Severe reduction in retinal sensitivity
- Severe constriction of isopters, absolute defects within 3 degrees of fixation
- Loss of central acuity
- Temporal island
Advanced Damage — Optic Nerve
- Diffuse enlargement of the optic cup
- Wipe out of all or a portion of the neuroretinal rim
Normal-tension glaucoma is a diagnosis of exclusion. If the doctor investigates thoroughly, most cases of normal-tension glaucoma can be correctly ascribed to another disease.
Differential diagnosis will depend on if the damage is observed on the optic nerve or a visual field defect is present. Below is a list of possible differential diagnosis.
Optic Nerve Head
- Congenital and hereditary anomalies of the disc
- Ischemic optic neuropathy
- Compressive lesions of the optic nerve
- Optic nerve hypoplasia
- Tilted discs
Visual Field Defect
- Pituitary tumors
- Ischemic optic neuropathy
- Hypovolemic optic neuropathy
- Non-glaucomatous optic neuropathy
- Arteritic and non-arteritic anterior ischemic optic neuropathy
- Burnt-out primary open-angle glaucoma
- Vascular disease
- Chronic angle-closure glaucoma
- Drusen of the optic nerve
- Intraocular pressure-lowering systemic medications, such as beta blockers for hypertension
- Abnormally thin cornea masking true ocular hypertension
- 70 um change in corneal thickness can approximate 5 mm Hg of intraocular pressure
- Neurological condition
When initiating treatment, assume that the pre-treatment measurement of intraocular pressure (IOP) is the level that produced damage to the optic nerve. If the IOP remained at this level, additional damage to the optic nerve would follow.
To treat glaucoma, an IOP level is identified below which further optic nerve damage is unlikely to occur. This IOP level is the target pressure range and it is selected based on the following:
- Pre-treatment level of IOP
- The rapidity with which the damage to the optic nerve occurred, if that is known
- Patient age
- General health of the patient
Treatment should maintain the IOP at or below the target level. The status of the optic nerve, visual fields, electrodiagnostics, and the retinal nerve fiber layer are monitored over time for evidence of stability or deterioration. In the event of further damage, the target pressure range is reset to a lower level.
Pharmacologic Treatment
Select your initial medication based upon target pressure range, medical history, and ocular history. If the initial medication fails to achieve the target pressure range within one month, discontinue the initial medication and substitute another.
If the second medication fails to achieve the target pressure, begin combination therapy by using two different medications. If this strategy fails, you could add still a third class of glaucoma medications to the regimen. With three different eyedrops, non-compliance becomes common and laser surgery may be a better treatment option.
Prostaglandins are the most popular class of medications for glaucoma therapy due to their excellent efficacy, safety index and tolerability. They flatten the diurnal curve significantly and achieve the greatest IOP reduction of any class of topical medication.
Classes of Glaucoma Medications
Prostaglandins
- Lumigan
- Travatan Z
- Zioptan
- Xalatan
Beta-Blockers
- Timolol
- Betagan
- Betimol
- OptiPranolol
Adrenergic Agonists
- Alphagan P 0.1% and 0.15%
- Brimonidine 0.2%
- Propine
Carbonic Anhydrase Inhibitors
- Azopt
- Trusopt
Cholinergic Agonists
- Pilocarpine
- Carbachol
- Echothiophate
Docosanoids
- Rescula
Combination Glaucoma Medications
- Cosopt – carbonic anhydrase inhibitor / beta-blocker
- Cosopt PF – carbonic anhydrase inhibitor / beta-blocker
- Combigan – adrenergic agonist / beta-blocker
- Simbrinza – adrenergic agonist / carbonic anhydrase inhibitor
Changing the Treatment due to Side Effects
Prostaglandins
- Red eye
- Eye color change
- Excessive eyelash growth
- Uveitis
- Macular edema
Beta-Blockers
- Bronchospasm
- Pulmonary edema
- Heart failure
- Headache
- Weakness
- Depression
- Lethargy
- Itching
- Stinging
- Blurred vision
- Photophobia
- Loss of libido
Adrenergic Agonist
- Red eye
- Allergic follicular conjunctivitis
- Dry mouth
- Drowsiness
Carbonic Andydrase Inhibitors
- Sulfa allergy
- Red eye
- Ocular itching
- Metallic taste
- Paresthesia of fingers or toes
- Headache
- Blood dyscrasias
- Depression
- Loss of libido
- Impotence
Cholinergic Agonists
- Red eye
- Induced myopia
- Reduced vision in low illumination
- Headaches
- Lens opacities
- Iris cysts
- Increased risk of angle closure
- Increased risk of retinal detachment
- Sweating
- Salivation
- Diarrhea
- Bradycardia
- Dyspnea
Docosanoids
- Eye color change
- Stinging
- Increase in periocular eyelid pigmentation
- Increase in upper eyelid sulcus deepening
1. Dada T, Kumar G, Mishra SJ. Ultrasound Biomicroscopy in Glaucoma: An Update. Journal of Current Glaucoma Practice. January 2008.
2. Al-Aswad L, Tsai J. Managing the Narrow-Angle Patient. RevOphth. 30 June 2004. http://www.revophth.com/content/i/1330/c/25527/. Last accessed May 30, 2014.
3. Sowka J. Normal-Tension Glaucoma. http://optometry.nova.edu/~jsowka/Course_Notes/Normal%20Tension%20Glaucoma.doc. Last accessed June 11, 2015.
4. Ventura LM, Golubev I, Feuer W, Porciatti V. The PERG in Diabetic Glaucoma Suspects With No Evidence of Retinopathy. J Glaucoma 2010; 19(4): 243-247.
5. Tsai JC. VEP Technology for the Detection of Glaucomatous Visual Field Loss. Glaucoma Today. 2009 March. http://glaucomatoday.com/2009/03/GT0309_10.php/. Last accessed June 25, 2015.
6. Banitt M, Ventura L, Feuer W, Savatovsky E, Luna G, Shif O, Bosse B, Porciatti V. Progressive Loss of Retinal Ganglion Cell Function Precedes Structural Loss by Several Years in Glaucoma Suspects. National Institutes of Health-National Eye Institute. 7 Feb 2013. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3626526/. Last accessed June 25, 2015.
7. Malik R, Swanson W, Garway-Teath D. The ‘Structure-function’ Relationship in Glaucoma — Past Thinking and Current Concepts. Clin Experiment Ophthalmol. 2012 May-Jun;40(4):369-80. doi: 10.1111/j.1442-9071.2012.02770.x. Epub 2012 Apr 12. http://www.ncbi.nlm.nih.gov/pubmed/22339936. Last accessed June 29, 2015.
8. Bremmer F.D. Pupil Assessment in Optic Nerve Disorders. Eye (Lond). 2004 Nov;18(11):1175-81. http://www.ncbi.nlm.nih.gov/pubmed/15534603. Last accessed June 29, 2015.
9. Chew S, Cunningham W, Gamble G, Danesh-Meyer H. Retinal Nerve Fiber Layer Loss in Glaucoma Patients with a Relative Afferent Pupillary Defect. Invest Ophthalmol Vis Sci. 2010 Oct;51(10):5049-53. doi: 10.1167/iovs.09-4216. Epub 2010 May 5. http://www.ncbi.nlm.nih.gov/pubmed/20445112. Last accessed June 29, 2015.
10. Tielsch JM, Sommer A, Katz J, Royall RM, Quigley HA, Javitt J. Racial Variations in the Prevalence of Primary Open-Angle Glaucoma The Baltimore Eye Survey. JAMA. 1991 Jul 17;266(3):369-74. http://www.ncbi.nlm.nih.gov/pubmed/2056646. Last accessed June 29, 2015.
11. Rabin J, Gooch J, Ivan D. Rapid Quantification of Color Vision: The Cone Contrast Test. Invest Ophthalmol Vis Sci. 2011 Feb 9;52(2):816-20. doi: 10.1167/iovs.10-6283. http://www.ncbi.nlm.nih.gov/pubmed/21051721. Last accessed June 29, 2015.
365.12
Low tension open-angle glaucoma
92133
Retinal nerve fiber laser scan
92083
Visual field examination
92250
Fundus photography
92225
Extended ophthalmoscopy
92226
Subsequent ophthalmoscopy
92020
Gonioscopy
95930
Visual evoked potential
92275
Electroretinography
92100
Serial tonometry
92132
Anterior segment imaging
76513
Anterior segment ultrasound
76514
Corneal pachymetry
Occurrence
The prevalence of open-angle glaucoma is almost 2% of the population over 40 years old.
Distribution
Glaucoma is not distributed evenly throughout the population.
- Black Americans 4 to 5 times more likely to develop glaucoma
- More women than men develop glaucoma
- Latino Americans have very high risk in advanced age
Risk Factors
- Vertically elongated cup-to-disc ratios
- Asymmetric cup-to-disc ratios
- Intraocular pressures greater than 21 mmHg
- Myopia
- Advancing age
- Black or Latino race
- Thin corneas
- Disc hemorrhages
- Vascular disease
- Family history
- Medical history
- Carotid insufficiency
- Cardiovascular disease
- Empty sella syndrome
- Abnormal blood coagulation and platelets




 Print | Share
Print | Share