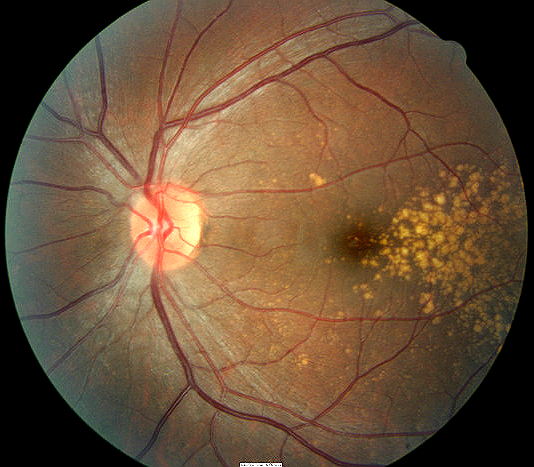
Degenerative drusen temporal to the macula
ICD-10 Diagnosis Codes:
H35.361–Drusen (degenerative) of macula, right eye
H35.362–Drusen (degenerative) of macula, left eye
H35.363–Drusen (degenerative) of macula, bilateral
Title
Drusen (Degenerative) Of Retina
Category
Other Retinal Disorders
Description
Degenerative drusen also called familial or dominant drusen is an asymptomatic, bilateral, symmetric, yellow-white nodular thickening of the retinal pigment epithelium basement membrane.
Degenerative drusen is an asymptomatic, bilateral, symmetric, yellow-white nodular thickening of the retinal pigment epithelium. Over time, the lesions may coalesce and form a honeycomb appearance, or they can enlarge. Drusen are often associated with pigment clumping, chorioretinal atrophy and choroidal neovascular membrane (CNVM). The onset of clinical signs may be seen by age 20-30 years. The onset of clinical symptoms occurs in the third to fourth decade of life and may involve an associated exudative or non-exudative retinal detachment, at the level of the retinal pigment epithelium.
Structural Damage to the Eye
- Separation of sensory retinal tissue to underlying retinal pigment epithelium and choroid due to holes, tears or breaks
- Accumulation of subretinal fluid in inappropriate places
- Traction from inflammatory or vascular fibrous membranes causes adhesions between the vitreous gel and the retina leading to detachments
Functional Damage to the Eye
- Decreased vision
- Associated visual field defects to corresponding areas of choroid, retinal or chorioretinal detachments or tears.
- Permanent vision loss with complications from choroidal neovascular membranes
The main goal of the diagnostic evaluation in a patient with degenerative drusen is to accomplish the following:
- Identify the location and extent of the drusen
- Educate the patient on the genetic component of the condition
- Monitor the progression over time
Patient History
Patients will present with the following symptoms or signs:
- Asymptomatic initially or progressive decreased vision
- Associated gross visual field defects
Clinical Appearance of the Retina
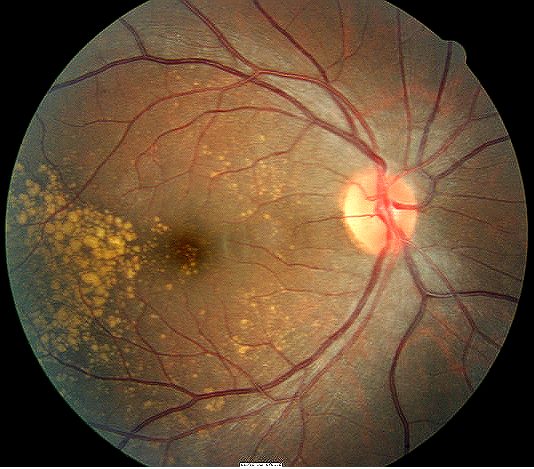
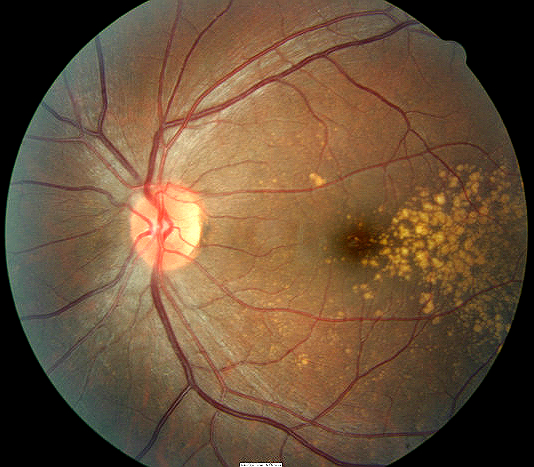
- Look for bilateral, symmetric, yellow-white drusen which is nodular thickening of the retinal pigment epithelium basement membrane
- Look for complications of choroidal or retinal detachments/tears and choroidal neovascular membranes
 |
 |
DIAGNOSTIC TESTS
The goal of the following tests is to accomplish the following:
- Document the extent and location of the drusen
- Determine the structural and functional damage to the eye
- Assist in monitoring the drusen for progression
Refraction
- Measurement of visual function / visual acuity
Extended Ophthalmoscopy
- Evaluate retinal morphology
- Document abnormal structural changes to the maucla and retina
- Evaluate for any abnormal retinal thinning, tears or detachments
- Evaluate for the presence of choroidal neovascular membrane
Fundus Photography
- Evaluate and document abnormal retinal and macular changes
Retinal Scanning Laser
- Evaluate and document abnormal retinal and macular changes
No specific classification is in place for degenerative drusen
Age-Related Macular Degeneration
Age-related macular degeneration (ARMD) will also form drusen in the posterior pole, but this drusen is a focal collection of eosinophilic homogenous material lying between the basement membrane of the retinal pigment epithelium and the collagenous portion of Bruch’s membrane. The retinal drusen associated with age-related macular degeneration shows up later in life versus degenerative drusen which begins to appear between 20-30 years of age.
There is no treatment for degenerative drusen.
- If complications arise from the drusen, they are treated according to the cause
- Routinely monitor patients for choroidal neovascularization membrane (CNVM) formation and choroidal/retinal detachments
- Extrafoveal or juxtafoveal CNVM can be treated with laser photocoagulation or intravitreal anti-VEGF injections
- Symptomatic retinal breaks can be treated with laser photocoagulation, cryotherapy or scleral buckling surgery
1. Fong D. Age-Related Macular Degeneration: Update For Primary Care. Am Fam Physician. 2000 May 15;61(10):3035-3042. http://www.aafp.org/afp/2000/0515/p3035.html. Last accessed August 17, 2014.
362.57
Drusen (degenerative) of retina
92250
Fundus photography
92225
Extended ophthalmoscopy
92134
Macula OCT scan
92083
Visual field examination
92275
Electroretinography
92283
Color vision examination
Occurrence
Degenerative drusen is not very common in the population.
Distribution
Degenerative drusen is distributed evenly throughout the population.
Risk Factors
Autosomal dominant pattern of inheritance.




 Print | Share
Print | Share