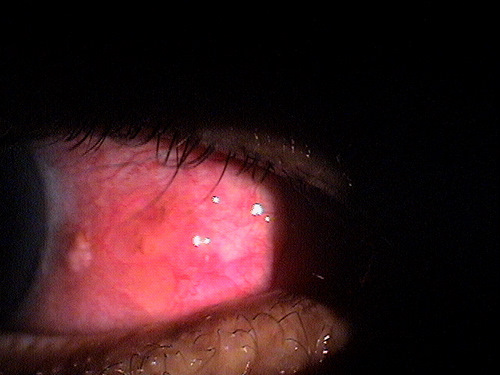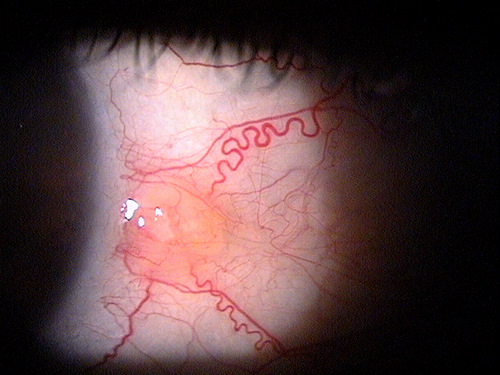
Clinical appearance of a pinguecula during
an episode of pingueculitis
ICD-10 Diagnosis Codes:
H10.811–Pingueculitis, right eye
H10.812–Pingueculitis, left eye
H10.813–Pingueclitis, bilateral
Title
Pingueculitis
Category
Disorders Of The Conjunctiva
Description
Pingueculitis is the inflammation of a pre-existing pinguecula.
Pingueculitis is an inflammation of a pre-existing pinguecula. A pinguecula is a type of conjunctival degeneration that forms as a result of an elastic and collagen degenerative process. Pinguecula formation is believed to be precipated by ultraviolet light and environmental exposure. Advancing age is also a risk factor in the development of a pinguecula.
The images below present a normal pinguecula upon initial examination and again 10 months later during an episode of pingueculitis:
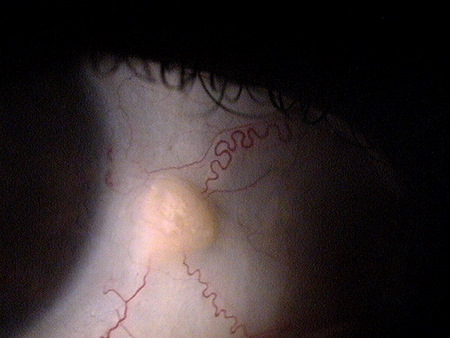 |
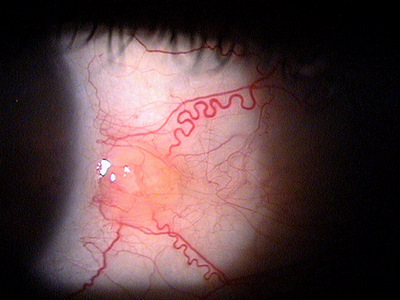 |
There are several types of initiating insults that result in pingueculitis.
Mechanical irritation by the eyelids during the blink mechanism
- This mechanical irritation occurs when the pinguecula becomes abnormally elevated or abnormally sized, and the eyelids have trouble moving over the lesion.
Improperly fitting contact lenses
- This occurs when the diameter of the contact lens is not appropriate for the size or location of the pingeucula and the edge of the contact lens irritates the lesion.
Exposure to environmental irritants
- UV radiation and environmental irritants such as dust or debris produce chronic irritation that draws inflammatory cells to the pinguecula, and the inflammatory response begins.
Ocular surface disease
Moderately severe dry eye syndrome and chronic ocular allergy can produce chemical irritation and structural damage to the ocular surface. When this irritation and damage is localized on or around a pre-existing pinguecula, pingueculitis may result.
Structural Damage to the Eye
|
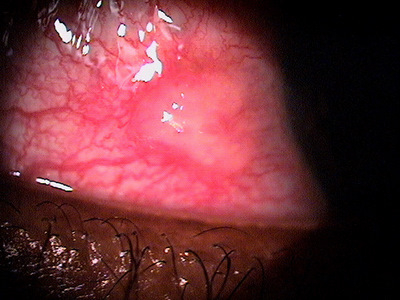 |
The main goal of the diagnostic evaluation of a patient with pingueculitis is to accomplish the following:
- Determine the initiating insult
- Classify the disease
- Prescribe a treatment plan
Patient History
Patients with pingueculitis will usually present with the following signs and symptoms.
- Red eye
- Ocular discomfort
Clinical Appearance of the Conjunctiva
- Interpalpebral conjunctival mass or lesion
- Localized conjunctival hyperemia
- Exposure keratoconjunctivitis
- Punctate epithelial erosions of the conjunctival epithelium
- Corneal delle
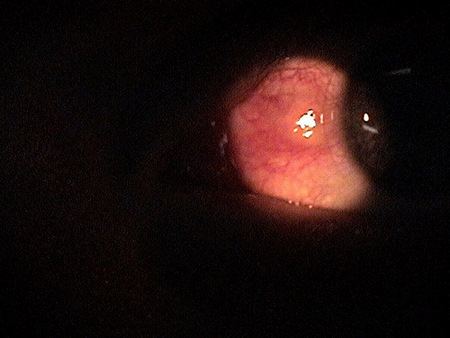 |
Pingueculitis
|
|
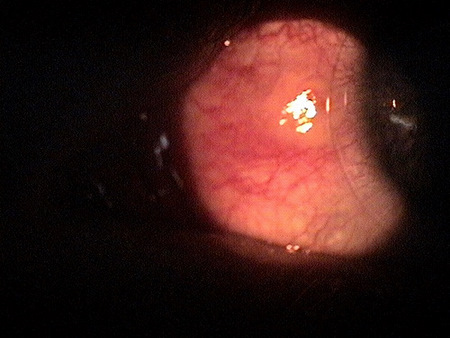 |
Pingueculitis
|
|
Pingueculitis
|
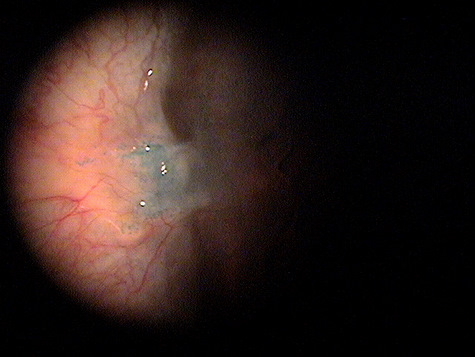 |
|
Exposure Keratoconjunctivitis
|
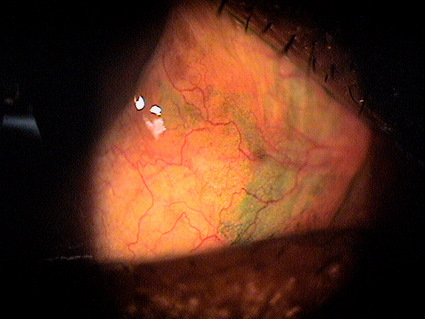 |
|
Corneal Delle
|
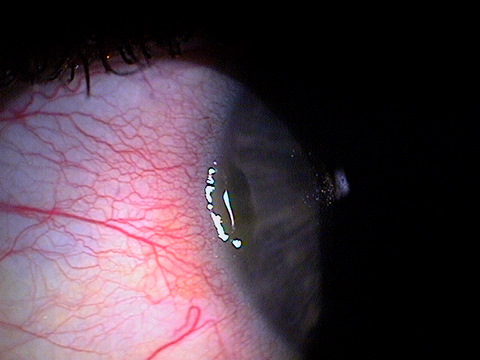 |
DIAGNOSTIC TESTS
External Ocular Photography
- Document the size and shape of the pinguecula
- Document any damage to the ocular surface from the pinguecula
- Document any changes in size and shape of the pinguecula
- Document any changes in the cornea or conjunctiva
- Help develop a treatment plan
|
|
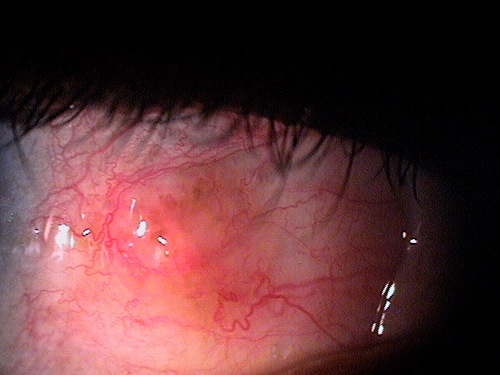 Day 3 – Pingueculitis improving |
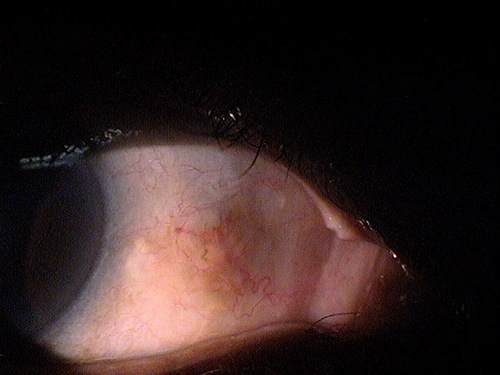 Day 8 – Pingueculitis resolved |
Pingueculitis is classified based upon its initiating insult.
- Abnormal pinguecula height or size
- Improperly fitted contact lenses
- Exposure to environmental irritants
- Ocular surface disease
This would include any other disease that presents as an interpalpebral conjunctival mass or elevation. Conjunctival lesions with this clinical appearance may be also a clinical sign of the following diseases or conditions. If conjunctival hyperemia is present, the location of the hyperemia, its time of onset, the severity of any ocular discomfort, and the determination of an initiating insult are all important factors to consider when excluding any of the following differential diagnoses.
- Episcleritis
- Scleritis
- Conjunctival retension cyst
- Limbal follicle
- Pseudoepitheliomastous hyperplasia
- Conjunctival intraepithelial neoplasia
- Conjunctvial dermoid
- Chlamydial infection
- Chemical or thermal injury
The treatment of pingueculitis is determined by the etiology of the disease. Because pingueculitis is an inflammatory condition, topical anti-inflammatory medication will usually hasten the resolution of patient symptoms and clinical signs.
Pharmocologic Treatment
- Pingueculitis secondary to abnormally elevated or sized lesions usually responds to artificial tears and topical steroids. Treat the condition until the inflammation has resolved. Maintenance therapy may be required in some cases.
- Pingueculitis due to exposure to environmental irritants requires the identification and removal of the source of irritation (if possible), and then treat the inflamed pinguecula with lubrication and topical steroids until the inflammation has resolved.
- Pingueculitis associated with ocular surface disease requires that the associated condition be diagnosed and treated along with the specific treatment for the inflamed pinguecula.
Contact Lens Treatment
Pingueculitis secondary to improperly fitted contact lenses requires the prescription of a contact lens with a different diameter and/or base curve. Artificial tears and topical steroids are helpful in the initial phase of treatment.
Surgical Treatment
In extreme cases, when long-term pharmocologic treatment has been unsuccessful, surgical excision of the pinguecula may be required.
Preventive Treatment
Prevention of pingueculitis involves the following activities and recommendations:
- Wearing eyeglasses with an ultraviolet filter
- Treating pre-existing ocular surface disease
- Avoiding environmental irritants
- Excluding some patients with pre-existing pinguecula from wearing contact lenses
1. Abelson MB, Mertz P. Pingueculitis: how to keep your patients safe from this condition. Review of Cornea & Contact Lenses. Sept. 2006: 8.
2. Pingueculitis. RevOptom. Handbook of ocular disease management. http://legacy.revoptom.com/handbook/sect2h.htm. Last accessed March 31, 2014.
3. Prince M. Pingueculitis A.K.A. “Inflamed Pinguecula.” http://myeyepod.blogspot.com/2011/04/pingueculitis-aka- inflamed-pinguecula.html. Last accessed March 31, 2014.
4. Fisher J. Pterygium. Medscape. 17 April 2013. http://emedicine.medscape.com/article/1192527- overview#a0199. Last accessed July 22, 2014.
372.34
Pingueculitis
92285
External ocular photography
Occurrence
Occurrence within the general population varies with geographical location.
- Within the continental United States, prevalence rates vary from less than 2% above the 40th parallel to 5-15% in latitudes between 28-36°
- A relationship is thought to exist between increased prevalence and elevated levels of ultraviolet light exposure in the lower latitudes
Distribution
- Pingueculitis is reported to occur in males twice as frequently as in females
- Patients over 40-years-old have the highest prevalence
Risk Factors
- Sex
- Age
- UV-B exposure
- Outdoor activities




 Print | Share
Print | Share