ICD-10 Diagnosis Codes:
H18.421 — Band keratopathy, right eye
H18.422 — Band keratopathy, left eye
H18.423 — Band keratopathy, bilateral
Title
Band Keratopathy
Category
Corneal Opacity And Other Disorders Of Cornea
Description
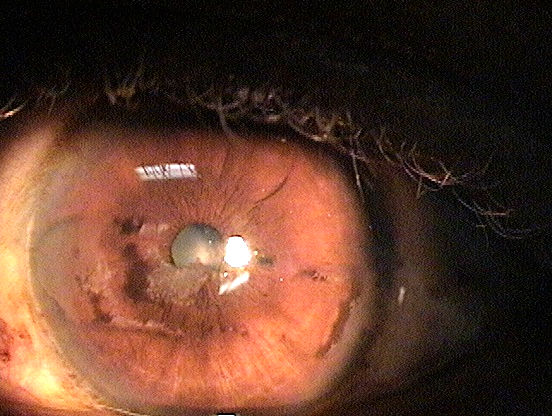
Band keratopathy is a corneal disease derived from the appearance of calcium on the central cornea.
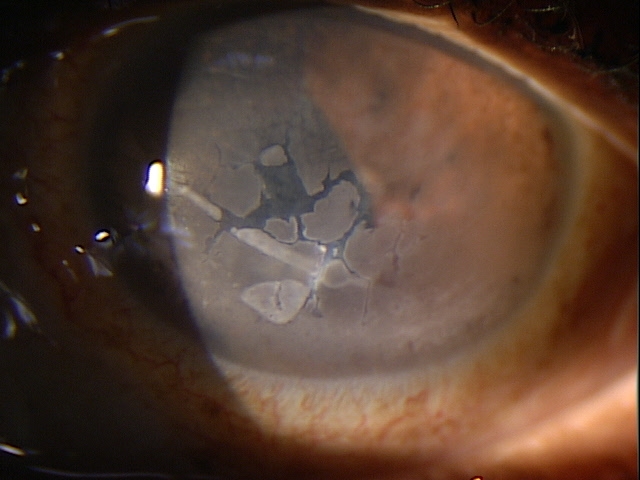
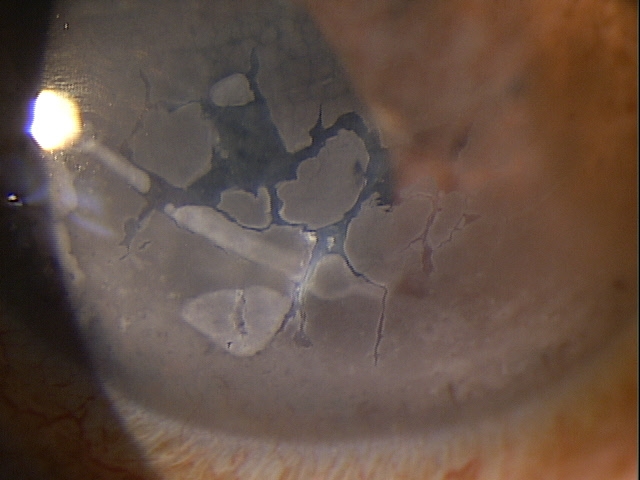
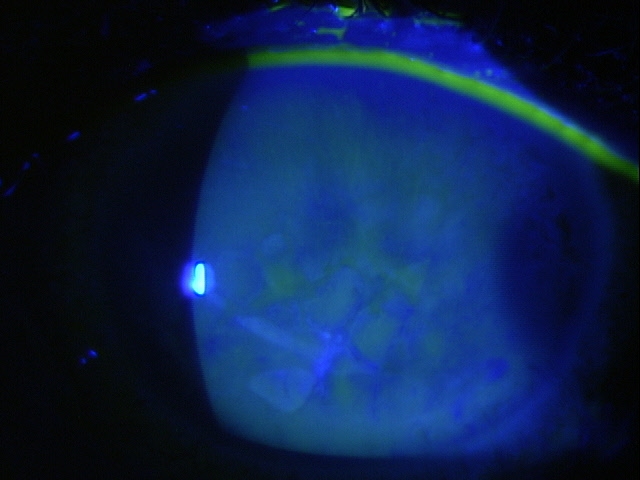
Band keratopathy is characterized by the appearance of a band across the central cornea, formed by the precipitation of calcium salts on the corneal surface (directly under the epithelium). This form of corneal degeneration can result from a variety of causes, either systemic or local, with visual acuity decreasing in proportion to the density of the deposition.
 |
 |
 |
Structural Damage to the Eye
- xxxx
- xxxx
Functional Damage to the Eye
- Decreased vision
- Foreign body sensation
- Ocular irritation
- Redness
The main goal of the diagnostic evaluation in a patient with band keratopathy is to accomplish the following:
- Determine the underlying condition producing the band keratopathy
- Relieve ocular discomfort
- Prevent complications that occur with epithelial defects (i.e., infection, uveitis)
- Improve visual acuity
Patient History
Patients will usually present with the following symptoms and/or clinical history:
- Blurred vision
- Eye pain
- Foreign body sensation
- Sensitivity to bright light
- Epiphora
- History of pre-existing corneal disease
- History of previous ocular surgery (especially cataract surgery)
External Ocular Examination with Biomicroscopy
- Loss of stromal transparency
- Folds in Descemet’s membrane
- Obvious thickening of the cornea
- Epithelial blisters and bullae
- Loss of corneal luster
I am text block.
Conditions to consider in the differential diagnosis of band keratopathy include the following:
- Gout
- Interstitial keratitis
- Primary and secondary calcareous degeneration of the cornea
- Calciphylaxis — An ocular and systemic hypersensitivity reaction characterized by calcium deposition in response to specific antigens or agents
- Spheroidal degeneration — Bandlike deposition of hyaline
The goals of pharmacotherapy are to reduce plasma calcium levels, to prevent complications, and to reduce morbidity.
Superficial Debridement
Superficial debridement in band keratopathy is usually effective in restoring normal vision. Various adverse outcomes can result from the procedure, including corneal scarring and vision loss, but the incidence of such complications is very low.
Although medical therapy is ineffective in treating band keratopathy, underlying conditions associated with elevated levels of calcium or phosphate should be treated to prevent deposition from recurring.
Chelation Therapy
If the patient only experiences mild foreign body sensation with no effect on vision, treating with topical lubrication—as you would treat ocular surface disease—may suffice. As the patient progresses to visual acuity loss, increased foreign body sensation or increased cosmetic concerns, further intervention is warranted. The recommended course is chelation by disodium ethylenediaminetetraacetic acid (EDTA).
In the chelation procedure, the cornea is prepped by gentle epithelial debridement with a spud or scalpel, then a corneal well is placed on the eye and disodium EDTA 3% is added to it. The solution alone will dissolve the calcium precipitates, but gentle rubbing of the plaques increases the break-up time. Once completed, the EDTA is rinsed off the cornea and a bandage contact lens is inserted for comfort until the cornea is re-epithelialized.
Diet
As noted, excessive vitamin D intake has been associated with band keratopathy, as has milk-alkali syndrome. Excessive absorption and serum elevation of calcium is the consequence of these 2 diet-related problems.
1. Taravella M. Band Keratopathy. Medscape/EMedicine. 1 May 2014. http://emedicine.medscape.com/article/1194813-overview. Last accessed August 9, 2015.
2. Claypool C, Sturbaum C. Band on the Run. RevOptom. 15 April 2014. http://www.reviewofoptometry.com/content/d/surgical_minute/i/2823/c/50883/. Last accessed August 11, 2015.
371.43
Band-shaped keratopathy
Band keratopathy treated with PROKERA amniotic membrane
Occurrence
Distribution
Risk Factors
Local ocular conditions associated with band keratopathy include the following:
-
Chronic uveitis
-
Juvenile idiopathic arthritis with uveitis
-
Phthisis bulbi
-
End-stage glaucoma
-
Anterior mosaic dystrophy
-
Neurotrophic keratitis
-
Chronic herpes simplex stromal keratitis
-
Herpes zoster keratitis
The following conditions are associated with hypercalcemia, a risk factor for band keratopathy:
-
Hyperparathyroidism
-
Excessive vitamin D intake
-
Renal failure
-
Hypophosphatasia
-
Milk-alkali syndrome
-
Paget disease
-
Sarcoidosis
Drug-associated calcium deposition can result from the following:
-
Steroid phosphate preparations
-
Pilocarpine-containing, mercury-based preservatives
-
Viscoelastic agents – Rare, early formulations; may be related to phosphate buffers
-
Silicone oil
-
Topical medications containing phosphate buffers – Especially in the setting of chemical eye burns
-
Intraocular use of tissue plasminogen activator
Chemical fume ̶ related risk factors include the following:
-
Mercury vapor
-
Calcium bichromate vapor




 Print | Share
Print | Share