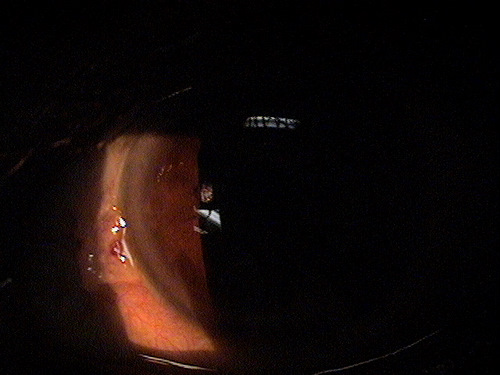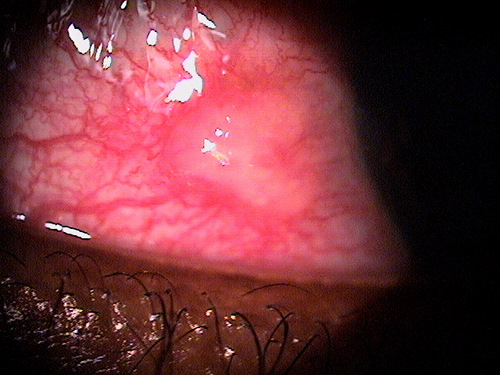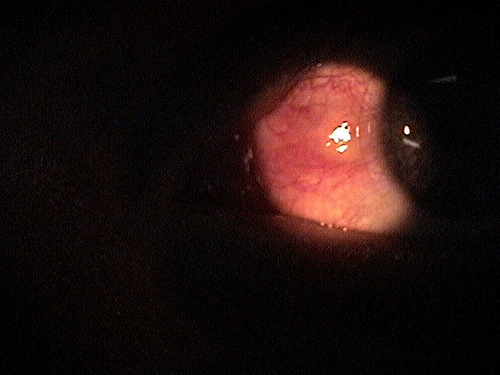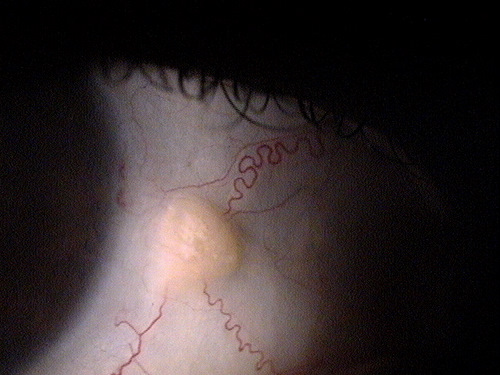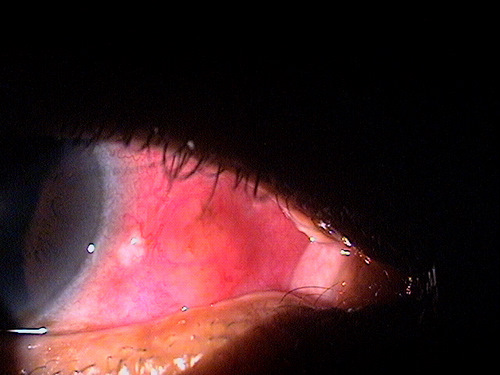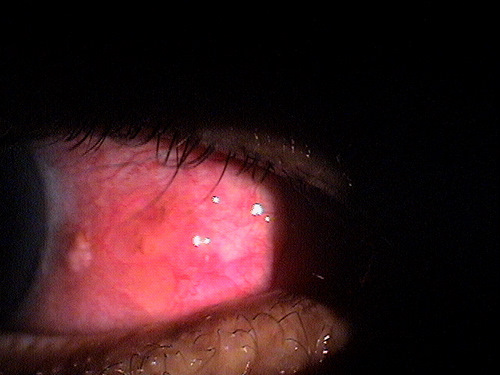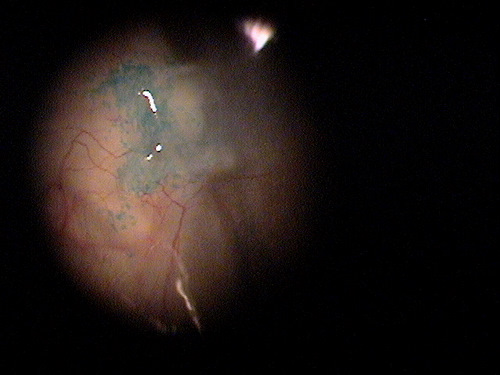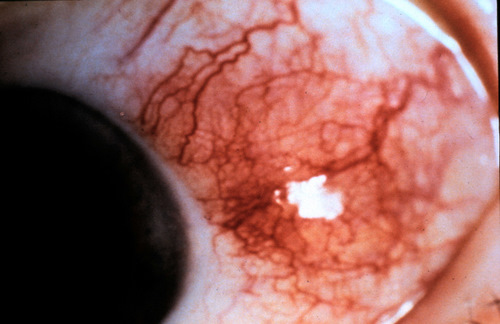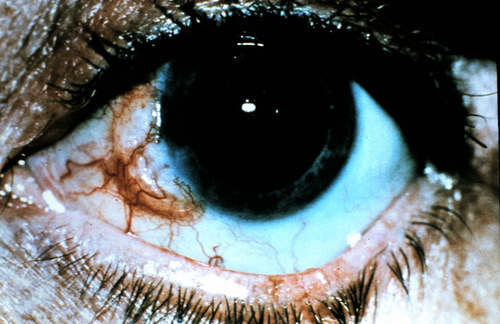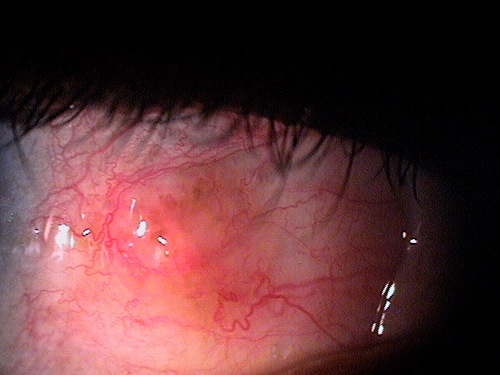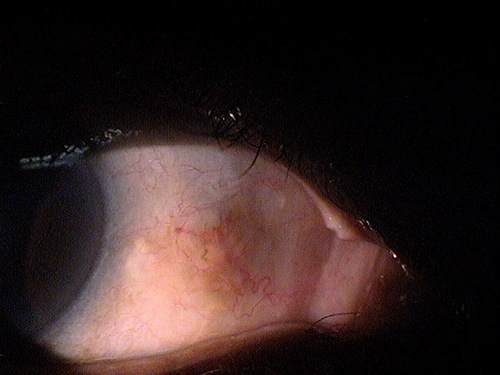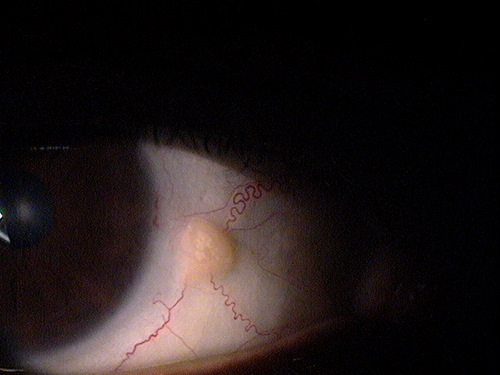
Small non-inflamed pinguecula
ICD-10 Diagnosis Codes:
H11.151–Pinguecula, right eye
H11.152–Pinguecula, left eye
H11.153–Pinguecula, bilateral
Title
Pinguecula
Category
Disorders Of The Conjunctiva
Description
A pingueculla is a type of conjunctival degeneration appearing as a yellow or white elevated superficial mass on the conjunctiva.
A pinguecula appears as a yellow-white elevated, superficial mass on the surface of the eye. Pinguecula are usually located in the interpalpebral fissure and they do not involve the cornea. Although pinguecula are very common and usually benigh, they may be associated with chronic exposure keratoconjunctivitis.
A pinguecula consists of an abnormal degeneration of the collagen fibers in the conjunctival stroma. There may be a thinning of the overlying conjunctival epithelium and some calcification within the body of the lesion. Pinguecula are found bordering the limbus on either side of the bulbar conjunctiva.
Functional Damage to the Eye
- Reduced visual acuity secondary to corneal damage in exposure keratoconjunctivitis
- Reduced visual acuity secondary to ocular inflammation in severe pingueculitis
The main goal of the diagnostic evaluation is to accomplish the following:
- Determine the initiating insult(s)
- Classify the disease
- Prescribe a treatment program
Patient History
- Patient will come in and report a yellow “growth” on the surface of the eye
- If the patient has pingueculitis, they will come in with a red and irritated eye
DIAGNOSTIC TESTS
External Ocular Photography
- Document size and shape of the pinguecula
- Document any damage to the cornea from the pinguecula
- Document any change in size and shape of the pinguecula
- Document any changes in the cornea
- Plan treatment of the pinguecula
Pinguecula can be classified by size, location, height, or etiology. Once a pre-existing pinguecula becomes inflamed, the condition is called pingueculitis and is classified by the associated condition that causes the inflammation.
Type 0 – Normal Pinguecula
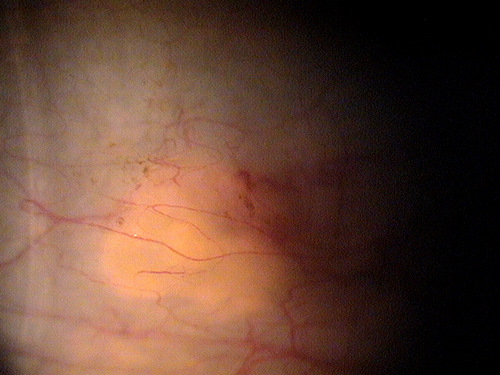 |
Normal Pinguecula
|
|
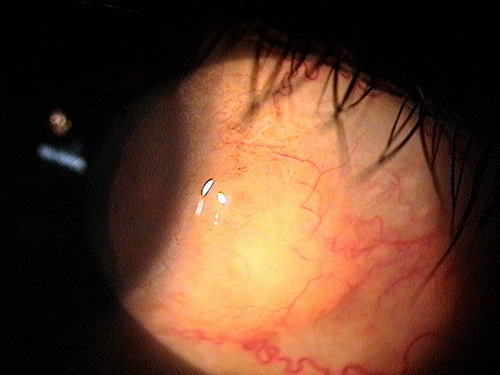 |
Normal Pinguecula
|
|
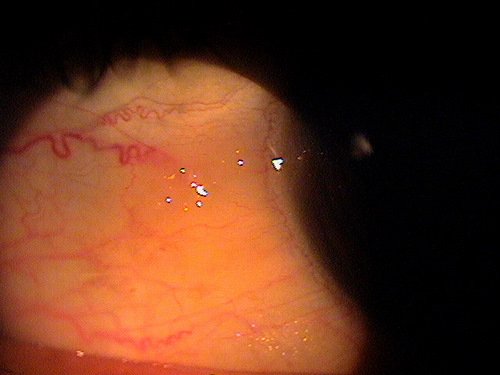 |
Normal Pinguecula
|
Type 1 – Pingueculitis secondary to abnormal lesion height or size
The most common initiating insult is mechanical irritation of the pinguecula by the eyelids during the blink mechanism. This mechanical irritation occurs when the pinguecula becomes abnormally elevated or abnormally sized, and the eyelids have trouble moving over the lesion. Since the eyelid margin has a significantly higher concentration of pain fibers than the conjunctiva, most patients will report the irritation as a foreign body sensation.
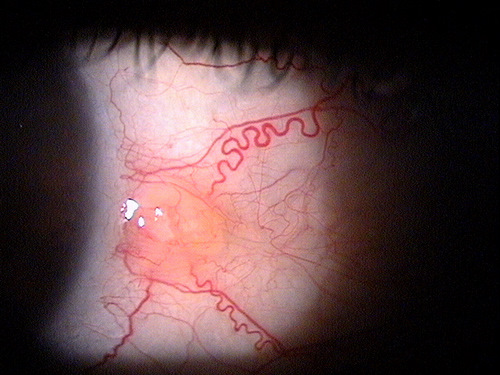
Mild pingueculitis |
Same lesion 10 months earlier |
Type 2 – Pingueculitis secondary to contact lens wear
If the pingueculitis is the result of a contact lens with a poor fitting relationship, discontinue contact lens wear, treat the inflamed pinguecula with lubrication and topical steroids, and if possible prescribe a contact lens with a different diameter or base curve.
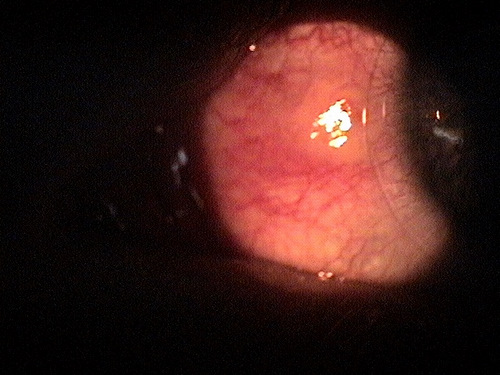 |
Contact Lens-Induced Pingueculitis
|
Type 4 – Pingueculitis secondary to ocular surface disease
Dry eye syndrome and chronic ocular allergy can produce chemical irritation and structural damage to the ocular surface. When this irritation and damage is localized on or around a pre-existing pinguecula, pingueculitis or pinguecula enlargement may occur. This type of pingueculitis has been implicated as a precursor of pterygium development.
This would include any other disease that present as an interpalpebral conjunctival mass or elevation. Lesions with this clinical apperance may also be a clinical sign of the following diseases or conditions:
- Episcleritis
- Scleritis
- Conjunctival retention cyst
- Limbal follicle
- Pseudoepitheliomastous
- Conjunctival dermoid
- Chlamydial infection
- Chemical or thermal injury
- Cervical interepithelial neoplasm leading to squamous cell carcinoma
The location of the hyperemia, its time of onset, the severity of any ocular discomfort, and the determination of an initiating insult are all important factors to consider when excluding any of the differential diagnoses.
Patients with a normal pinguecula can be observed. If the pinguecula is small and stable, it is an option to leave it alone. To reduce the chance of pinguecula enlargement, pingeuculitis or pterygium development doctors may recommend preventative treatment.
Preventative Treatment
- Decrease excessive exposure to wind and sunlight (UV)
- Aggressively treat any coexisting ocular surface disease
- Discontinue contact lens wear
- Prescribe contact lenses that do not irritate a pre-existing pinguecula
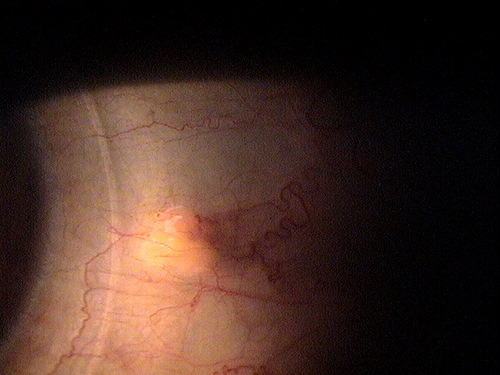 |
Contact Lens Patient
|
Pharmacologic Treatment
- Artificial tears
- Topical anti-inflammatory
Surgical Treatment
1. Abelson MB, Mertz P. Pingueculitis: how to keep your patients safe from this condition. Review of Cornea & Contact Lenses. Sept. 2006: 8.
2. Pingueculitis. RevOptom. Handbook of ocular disease management. http://legacy.revoptom.com/handbook/sect2h.htm. Last accessed March 31, 2014.
3. Prince M. Pingueculitis A.K.A. “Inflamed Pinguecula.” http://myeyepod.blogspot.com/2011/04/pingueculitis-aka- inflamed-pinguecula.html. Last accessed March 31, 2014.
4. Fisher J. Pterygium. Medscape. 17 April 2013. http://emedicine.medscape.com/article/1192527- overview#a0199. Last accessed July 22, 2014.
372.51
Pinguecula
92285
External ocular photography
Occurrence
Occurrence within the general population varies with geographical location.
- Within the continental United States, prevalence rates vary from less than 2% above the 40th parallel to 5-15% in latitudes between 28-36°
- A relationship is thought to exist between increased prevalence and elevated levels of ultraviolet light exposure in the lower latitude
Risk Factors
- Sex
- Age
- UV-B exposure




 Print | Share
Print | Share